 [Lymphoepithelioma-like carcinoma (LELC). ИВЧСОчЛѓЧЧСООч ОЯСО = Gastric carcinoma with lymphoid stroma] - №ћ
[Lymphoepithelioma-like carcinoma (LELC). ИВЧСОчЛѓЧЧСООч ОЯСО = Gastric carcinoma with lymphoid stroma] - №ћ
Previous | Home | EndoTODAY | List | Next
 [Lymphoepithelioma-like carcinoma (LELC). ИВЧСОчЛѓЧЧСООч ОЯСО = Gastric carcinoma with lymphoid stroma] - №ћ
[Lymphoepithelioma-like carcinoma (LELC). ИВЧСОчЛѓЧЧСООч ОЯСО = Gastric carcinoma with lymphoid stroma] - №ћ

2025-7-12. Рп ГДСі ОЪДТ БЫОч. MALT ИВЧССО РЧСѕРИЗЮ РЧЗкЕШ СјЧрМК РЇОЯ.
* LELC СѕЗЪ И№РН РЇСњШЏГЛНУАцОЦЦВЖѓНК 8ШЃ БтАэ (PDF)
3. EBV positive LELC of the stomach
4. EBV negative LELC of the stomach
5. РгЛѓРћ ЦЏТЁ
6. Colon LELC
7. FAQs
8. References
 1. Introduction to lymphoepithelioma-like carcinoma (LELC)
1. Introduction to lymphoepithelioma-like carcinoma (LELC)
Lymphoepithelioma-like carcinoma(LELC)ДТ КёРЮЕЮОЯАњ СЖСїЧаРћРИЗЮ РЏЛчЧЯАэ, ИВЧСБИМК АЃСњРЛ АЁСј ЙЬКаШЕШ РЇСООчРдДЯДй. Epstein-Barr ЙйРЬЗЏНКПЭРЧ ПЌАќМКЕЕ О№БоЕЧАэ РжНРДЯДй. LELCРК НФЕЕ, РЇ, ДуАќ, ХИОз МБ, Цѓ, РкБУ, ЧЧКЮ ЕюПЁМ ЙпЛ§ЧеДЯДй.
РЇ LELCДТ РќУМ РЇОЯРЧ l-4%ИІ ТїСіЧЯДТЕЅ СЖБтРЇОЯРЧ АцПь IIa + IIcЧќРЬ ИЙРИИч СјЧрМК РЇОЯРЧ АцПь Borrmann type IV ЧќРЬ ИЙДйАэ ЧеДЯДй. КДИЎЧаРкЕщРК medullary carcinomaЗЮ КЮИЃБтЕЕ ЧеДЯДй. СЖБтРЇОЯРЧ ЧќХТЗЮ ГЊХИГЏ АцПьДТ РЯЙнРћРЮ СЖБтРЇОЯАњ ПЙШФАЁ КёНСЧЯГЊ СјЧрМК РЇОЯРЧ ЧќХТИІ УыЧв АцПь РЯЙнРћРЮ СјЧрМК РЇОЯПЁ КёЧЯПЉ ПЙШФАЁ ШЮОР ССРК АЭРИЗЮ ОЫЗССЎ РжНРДЯДй. СЁИЗЧЯ СООчРЧ ЧќХТЗЮ ГЊХИГЊДТ АцПьЕЕ РжОю СжРЧАЁ ЧЪПфЧеДЯДй. 85%ДТ EBV ОчМКРЮЕЅ, EBV РНМКРЮ АцПьДТ ЛѓДыРћРИЗЮ ПЙШФАЁ ГЊЛоДЯДй.
КДИЎ МвАп (https://www.pathologyoutlines.com/)
ПРЗЁЕШ РњГЮ ЧЯГЊ МвАГЧеДЯДй.
Lymphoepithelioma-like carcinoma of the stomach: a subset of gastric carcinoma with distinct clinicopathological features and high prevalence of Epstein-Barr virus infection (Hepatogastroenterology 1999)
METHODOLOGY: Of 379 patients with gastric adenocarcinoma, from 1993 to 1996, 6 of them with lymphoepithelioma-like carcinoma of stomach were retrospectively studied.
RESULTS: Five patients were females and one patient was male. Their age ranged from 51-75 years with a mean age of 61.5 years. Endoscopically, 2 patients were initially diagnosed as early gastric cancer and the other 4 were diagnosed as advanced gastric cancer. Three patients had tumors located in the lower third of the stomach, while the other three tumors were located in the middle and upper third. Two tumors invaded into the serosal layer and the other four lesions were confined at submucosal and muscular layers. Using the in situ hybridization method, all 6 patients (100%) had positive nuclear Epstein-Barr virus-encoded small RNA signals in the tumor cells but not in the surrounding lymphoid stroma and non-neoplastic gastric mucosa. Helicobacter pylori was found in 4 (66.7%) of the cases. The mean follow-up period of the 6 patients was 27 months. Five patients were free of the disease. Lymph node involvement and mesenteric implantation was noted in one patient in which cancer recurred 1 year after gastrectomy.
CONCLUSIONS: Lymphoepithelioma-like carcinoma of stomach in this study revealed a female predominance, preferential localization in the proximal part of the stomach, better prognosis, and a high association with Epstein-Barr virus infection.
Korean J Gastrointest Endosc 2010 - ЛяМКМПяКДПјПЁМ КИАэЧЯПДДј СѕЗЪ
2019Гт WHO КаЗљПЁ БтМњЕШ КДИЎ МвАп: lymphoepithelioma-like carcinoma is considered to be a distinct subtype of undifferentiated carcinoma. It is characterized by a sheet-like arrangement of large epitheloid cells with prominent nuclei and indistinct borders. The tumor is surrouded by a characteristic inflammatory infiltrate that is rich in lymphocyte and plasma cells.
 3. EBV positive lymphoepithelioma-like carcinoma. EBV ОчМК ИВЧСОчЛѓЧЧСООч ОЯСО
3. EBV positive lymphoepithelioma-like carcinoma. EBV ОчМК ИВЧСОчЛѓЧЧСООч ОЯСО
Depth of invasionРК SM3ПДНРДЯДй.

1. Location : upper third, center at cardia (Siewert III)
2. Gross type : Borrmann type 2
3. Histologic type : Medullary carcinoma (lymphoepithelioma-like carcinoma)
4. Histologic type by Lauren : indeterminate
5. Size : 2.2x2.2 cm
6. Depth of invasion : invades muscularis propria
7. Resection margin: free from carcinoma, safety margin: proximal 1.4 cm, distal 2 cm
8. Lymph node metastasis : no metastasis in 52 regional lymph nodes
9. Lymphatic invasion : not identified
10. Venous invasion : not identified
11. Perineural invasion : not identified
12. Result of in-situ hybridization: Epstein-Barr virus: Positive
СЖСїАЫЛчПЁМДТ poorly differentiated adenocarcinomaПДАэ EUSПЁМ SM invasionРЬ ЖбЗЧЧпНРДЯДй.
Stomach, subtotal gastrectomy:
. Early gastric carcinoma
1. Location : lower third, Center at proximal antrum and anterior wall
2. Gross type : EGC type IIc
3. Histologic type : lymphoepithelioma-like carcinoma
4. Histologic type by Lauren : mixed
5. Size : 1.8x1.4 cm
6. Depth of invasion : invades submucosa (sm3) (pT1b)
7. Resection margin: free from carcinoma, safety margin: proximal 1 cm, distal 8.7 cm
8. Lymph node metastasis : no metastasis in 34 regional lymph nodes (pN0)
9. Lymphatic invasion : not identified
10. Venous invasion : not identified
11. Perineural invasion : not identified
12. AJCC stage by 7th edition: pT1b N0
13. Epstein-Barr virus : positive
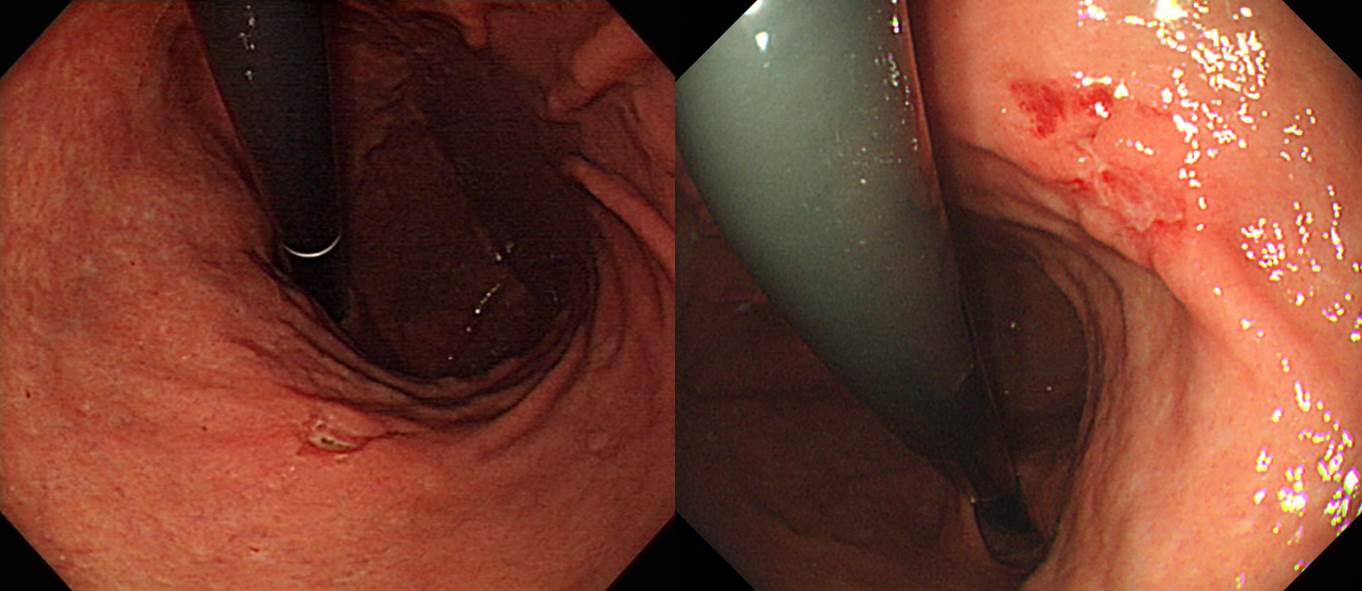
Stomach, subtotal gastrectomy:
. Early gastric carcinoma
1. Location : middle third, Center at body and posterior wall
2. Gross type : EGC type IIb
3. Histologic type : carcinoma with lymphoid stroma (medullary carcinoma)
4. Histologic type by Lauren : indeterminate
5. Size : 1.8x1 cm
6. Depth of invasion : invades submucosa (sm3) (pT1b)
7. Resection margin: free from carcinoma, safety margin: proximal 1.2 cm, distal 13 cm
8. Lymph node metastasis : no metastasis in 33 regional lymph nodes (pN0)
9. Lymphatic invasion : not identified
10. Venous invasion : not identified
11. Perineural invasion : not identified
12. AJCC stage by 7th edition: pT1b N0
2До АЃАнРИЗЮ 3Йј ГЛНУАц АЫЛчИІ ЙоРИМЬАэ, ИЖСіИЗ СЖСїАЫЛчПЁМ signet ring cell carcinomaАЁ ГЊПдНРДЯДй. УжСО КДИЎДТ carcinoma with lymphoid stromaЗЮ ГЊПдНРДЯДй. Lymphoepithelioma-like carcinomaЖѓАэ КЮИЃДТ ХИРдРдДЯДй. Lymphoid stroma ЛчРЬПЁ ЙЬКаШСЖСїЧќ РЇОЯРЬ ЙкЧєРжДТ ЧќХТРЬЙЧЗЮ, РАОШРћРИЗЮДТ SMT КёНСЧЯАд КИРЬАэ, СЖСїАЫЛчРЧ false negativeАЁ ИЙРК АЭ ААНРДЯДй.
Early gastric carcinoma
1. Location : lower third, Center at antrum and greater curvature
2. Gross type : EGC type IIc
3. Histologic type : carcinoma with lymphoid stroma
4. Histologic type by Lauren : mixed
5. Size : 3.8x1.9 cm
6. Depth of invasion : invades mucosa (muscularis mucosae) (pT1a)
7. Resection margin: free from carcinoma
8. Lymph node metastasis : no metastasis in 17 regional lymph nodes (pN0)
9. Lymphatic invasion : not identified
10. Venous invasion : not identified
11. Perineural invasion : not identified
12. AJCC stage by 8th edition: pT1a N0
Nasopharyngeal cancerЗЮ ФЁЗсЙоДј Сп PETИІ НУЧрЧЯПДДТЕЅ ПьПЌШї РЇОЯРЬ ЙпАпЕЧОю МіМњРЛ ЙоОвРН.
Stomach, subtotal gastrectomy: Early gastric carcinoma
1. Location : middle third, center at body and greater curvature
2. Gross type : EGC type I
3. Histologic type : lymphoepithelioma-like carcinoma
4. Histologic type by Lauren : intestinal
5. Size : 3.2x2.3x0.9 cm
6. Depth of invasion : extension to submucosa (sm2) (pT1b)
7. Resection margin: free from carcinoma, safety margin: proximal, 3.2 cm; distal, 8.8 cm
8. Lymph node metastasis : no metastasis in 36 regional lymph nodes (pN0) (0/36: lesser curvature, 0/10; greater curvature, 0/9; "1", 0/2; "3", 0/1; "4sb", 0/0; "5", 0/2; "6", 0/0; "7", 0/1; "8a", 0/2; "9", 0/6; "11p", 0/2; "12a", 0/1)
9. Lymphatic invasion : not identified
10.Venous invasion : not identified
11.Perineural invasion : not identified
 4. EBV negative lymphoepithelioma-like carcinoma. EBV РНМК ИВЧСОчЛѓЧЧСООч ОЯСО
4. EBV negative lymphoepithelioma-like carcinoma. EBV РНМК ИВЧСОчЛѓЧЧСООч ОЯСО
РгЛѓЛѓ Йз ГЛНУАц МвАп
65ММ ГВМКРЬ АЧСјГЛНУАцПЁМ ЙпАпЕШ РЇОЯ РЧНЩ МвАпРИЗЮ РЧЗкЕЧОњДй. СЖСїАЫЛч АсАњДТ Atypical cells, suspicious for poorly differentiated adenocarcinomaПДДй. ГЛНУАц РчАЫ(ПРИЅТЪ ЛчСј)ПЁМ РЇУМЧЯКЮ МвИИПЁ 4cm ХЉБтРЧ РЖБтЕШ КДМвАЁ РжОњАэ СпНЩКЮАЁ ЧдИєЕЧОю РжОњДй. РЬ КДМвРЧ БйРЇКЮРЮ РЇУМСпКЮПЁ Ию АГРЧ ИЖФЁ ЙЋД§Ањ КёНСЧб 1-3cm ХЉБтРЧ Ию АГРЧ РЖБтКЮАЁ РжОњДй. РЇУМЧЯКЮ ЧдИєРЛ ЕПЙнЧб РЖБтКЮ СЖСїАЫЛчДТ tubular adenocarcinoma, moderately differentiated (cytokeratin AE1/AE3 positive) ПДРИИч РЬКИДй БйРЇКЮ СЁИЗЧЯСООч РЏЛчЧб РЖБтКЮЕщРЧ СЖСїАЫЛчДТ gastritis ЛгРЬОњДй. МіМњРЛ НУЧрЧЯПДДй.
СјДм Йз АцАњ
EBV negative, lymphoepithelioma-like carcinoma. МіМњРхПЁМ subtotal gastrectomy АшШЙРИЗЮ РЇИІ ЧѲЧЯПДРИГЊ АЫУМ ШЎРЮ НУ proximal marginРЬ 1cm СЄЕЕПДРИИч НФЕЕРЇСЂЧеКЮПЭ АЁБюПі total gastrectomyЗЮ РќШЏЧЯПДДй. КДИЎ АсАњ advanced gastric cancer, lymphoepithelioma-like carcinoma, Lauren indeterminate, 5x8x4.8cm, penetrated subserosal connective tissue, resection margin negative, no lymph node metastasis out of 40РЬОњДй (AJCC 8th pT3NO). БЫОчКЮ РЬПмДТ СЄЛѓСЁИЗ ОЦЗЁЗЮ ГаАд ФЇРБРЛ КИПДДй. Epstein-Barr virus РНМКРЬОњДй.
ЧиМГ
Lymphoepithelioma-like carcinomaДТ СЖСїЧаРћРИЗЮ КёРЮЕЮОЯАњ РЏЛчЧЯАэ ИВЧСБИМК АЃСњРЛ АЁСј ЙЬКаШЕШ РЇСООчРИЗЮ SMT-like cancer Сп ЧЯГЊРЬДй. ПЙШФДТ РЯЙнРћРЮ РЇОЯКИДй ССДй. КЛ СѕЗЪУГЗГ EBV РНМКРЮ ПЙДТ ЛѓДыРћРИЗЮ ПЙШФАЁ ГЊЛкДй (Min. Gastric Cancer 2016).
 5. РгЛѓРћ ЦЏТЁ - (1) refractory ulcer, (2) lymphomaПЭ БИКаРЬ ОюЗЦДй
5. РгЛѓРћ ЦЏТЁ - (1) refractory ulcer, (2) lymphomaПЭ БИКаРЬ ОюЗЦДй
СІАЁ ДРГЂАэ РжДТ Ию АЁСі ЦЏТЁРЛ МвАГЧеДЯДй.
(1) Refractory ulcerРЧ РгЛѓЛѓРЛ КИРЯ Мі РжНРДЯДй. СЖСїАЫЛчРЧ false negativeАЁ ИЙДйДТ АЭАњЕЕ АќЗУЕШ ЦЏМКРдДЯДй. ОЦЗЁ СѕЗЪИІ КИНЪНУПР
Refractory ulcerЗЮ РЧЗкЕШ КаРдДЯДй. РЧЗк ШФ ГЛНУАц СЖСїАЫЛчПЁМ signet ring cell carcinomaАЁ ГЊПдНРДЯДй. МіМњ ШФ УжСО КДИЎДТ carcinoma with lymphoid stromaЗЮ ГЊПдНРДЯДй. Lymphoepithelioma-like carcinomaЖѓАэ КЮИЃДТ ХИРдРдДЯДй. Lymphoid stroma ЛчРЬПЁ ЙЬКаШСЖСїЧќ РЇОЯРЬ ЙкЧєРжДТ ЧќХТРЬЙЧЗЮ, РАОШРћРИЗЮДТ SMT КёНСЧЯАд КИРЬАэ, СЖСїАЫЛчРЧ false negativeАЁ ИЙРК АЭ ААНРДЯДй.
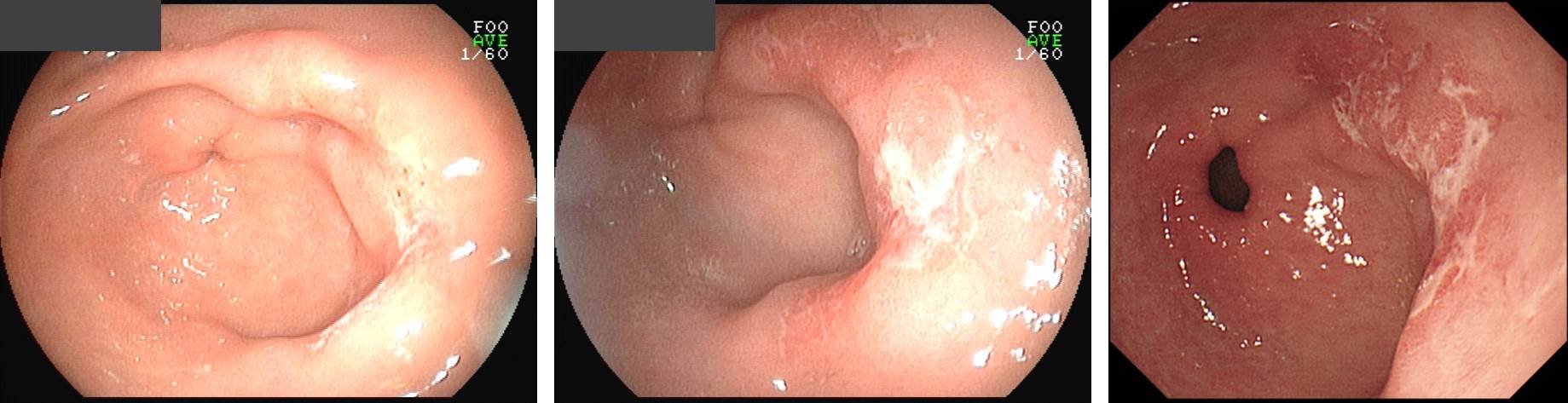
Early gastric carcinoma
1. Location : lower third, Center at antrum and greater curvature
2. Gross type : EGC type IIc
3. Histologic type : carcinoma with lymphoid stroma
4. Histologic type by Lauren : mixed
5. Size : 3.8x1.9 cm
6. Depth of invasion : invades mucosa (muscularis mucosae) (pT1a)
7. Resection margin: free from carcinoma
8. Lymph node metastasis : no metastasis in 17 regional lymph nodes (pN0)
9. Lymphatic invasion : not identified
10. Venous invasion : not identified
11. Perineural invasion : not identified
12. AJCC stage by 8th edition: pT1a N0
(2) MALT ИВЧССО РЧСѕРИЗЮ РЧЗкЕЧДТ АцПьАЁ РжНРДЯДй. СЖСїЧаРћ ЦЏТЁРЬ ЙЬКаШСЖСїЧќРЮ ОЯАњ МЏРЮ dense lymphoid infiltrationРЬЙЧЗЮ РлРК ГЛНУАц АтРк СЖСїПЁМДТ MALT ИВЧССОАњ ШЅЕПЕЩ Мі РжДТ АЭ ААНРДЯДй. ЕхЙААд АтРк СЖСїПЁМ moderately differentiatedРЮЕЅ УжСО КДИЎАсАњ LELCЗЮ ГЊПТ АцПьЕЕ РжНРДЯДй. ПЉЧЯЦА АтРк СЖСїПЁМ СјДмРЬ ОюЗСПю СЖСїЧќРдДЯДй. ОЦЗЁ ЕППЕЛѓРЛ КИНУБт ЙйЖјДЯДй.
2022Гт 3Пљ KASID БГРАРкЗс. МГИэ Сп ЧеЦїУМДТ syncytiumРЛ ИЛЧд (ММЦї РЖЧеРИЗЮ ГЊХИГЊДТ ДйЧйМК ММЦї)
[2024-7-17. ОжЕЖРк СњЙЎ]
Carcinoma with lymphoid stroma ЖѓАэ ЧпРЛ ЖЇ, lymphoid stromaАЁ ОѓИЖГЊ ИЙРИИщ РЬ СјДмРЬ КйДТ АЭРЮСі БУБнЧеДЯДй. КДИЎ РЧЛчРЧ СжАќРћРЮ ЦЧДмРЮ АЭРЮСі ОЦДЯИщ ИэШЎЧб БтСиРЬ РжДТСіПф?
[2024-7-17. Чб КДИЎ МБЛ§ДдРЧ ДфКЏ]
Lymphoid stromaРЧ percentage, ОчПЁ ДыЧб СЄРЧДТ ОјНРДЯДй. КДИЎРЧЛчРЧ СжАќРћ ЦЧДмРЬБтДТ ЧЯГЊ, lymphoid stromaЛг ОЦДЯЖѓ poorly formed glands Ею LELCРЧ КДИЎ МвАпРЬ uniqueЧЯБт ЖЇЙЎПЁ КДИЎРЧЛчАЃ СјДм РЯФЁЕЕДТ ГєРЛАЭ ААНРДЯДй. Дм, LELCРЧ ЦЏТЁРћ СЖСї МвАпРК submucosaРЬЧЯПЁМ Рп КИРЬБтЖЇЙЎПЁ Л§АЫПЁМРЧ СјДмРК ОюЗЦНРДЯДй.
1. EndoTODAY EBV-associated gastric cancer
2. LELC СѕЗЪ И№РН РЇСњШЏГЛНУАцОЦЦВЖѓНК 8ШЃ БтАэ (PDF)
3. Epstein-Barr virus АќЗУ РЇОЯ РЬКРРК. Korean J Helicobacter Up Gastrointest Res 2021 (PDF)
© РЯПјГЛНУАцБГНЧ ЙйИЅГЛНУАцПЌБИМв РЬСиЧр. EndoTODAY Endoscopy Learning Center. Lee Jun Haeng.